Diabetes and heart disease are closely connected conditions that often develop alongside each other because they share many of the same underlying risk factors and biological effects on the body. One of the most important links between them is high blood sugar, which over time can damage the lining of blood vessels. This damage triggers inflammation and encourages the buildup of fatty deposits inside the arteries, a process known as atherosclerosis. As plaque accumulates, the arteries gradually narrow and become less flexible, making it harder for blood to circulate efficiently throughout the body. When this happens, the heart must work harder to pump blood, increasing strain on the cardiovascular system. Over long periods, this combination of restricted blood flow and increased cardiac workload raises the risk of serious complications such as heart attacks and strokes. What makes this process particularly dangerous is that it develops slowly and silently, often without obvious symptoms in the early stages. Many people are unaware of the changes occurring inside their blood vessels until a significant blockage or cardiovascular event occurs, highlighting the importance of early awareness and prevention.
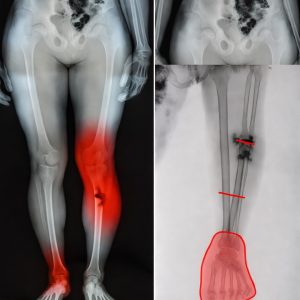
One of the earliest areas of the body where circulation problems tend to become noticeable is the feet. Because the feet are located farthest from the heart, they are more vulnerable to reduced blood flow when the circulatory system begins to deteriorate. Early warning signs in this area can include sensations of coldness, swelling, discoloration, or pain during walking or physical activity. These symptoms may seem minor at first, but they can indicate that blood is not reaching the lower extremities efficiently. Poor circulation in the feet is often one of the first visible indicators of broader vascular issues affecting the entire body. Recognizing these signs early is important because they can provide an opportunity to address underlying problems before they progress into more serious conditions. Unfortunately, these symptoms are sometimes dismissed as temporary discomfort or normal aging, allowing the underlying cardiovascular issues to continue developing unnoticed.
In people with diabetes, the situation becomes more complex due to a condition known as neuropathy, which involves nerve damage caused by prolonged high blood sugar levels. Neuropathy can reduce or completely dull sensation in the feet, making it difficult for individuals to feel pain, temperature changes, or injuries. This loss of sensation creates a dangerous situation where cuts, blisters, or sores may go unnoticed for extended periods. At the same time, reduced blood flow slows the body’s ability to heal these injuries, increasing the risk of infection and further complications. What might begin as a small, manageable wound can quickly escalate into a more serious medical issue if it is not detected and treated early. The combination of poor circulation and reduced sensation makes foot care especially critical for individuals with diabetes, as the normal warning signals that alert the body to injury are often weakened or absent.
Another important condition that connects diabetes and heart disease is peripheral artery disease (PAD), which occurs when arteries in the limbs become narrowed or blocked due to plaque buildup. PAD primarily affects the legs and can cause symptoms such as cramping or pain during walking, often referred to as intermittent claudication. This discomfort typically improves with rest but returns with activity, reflecting the reduced ability of blood vessels to supply oxygen to the muscles. In more advanced cases, PAD can lead to slow-healing sores, persistent pain, and visible changes in skin color or texture, such as paleness, bluish tones, or thinning skin. Because PAD is closely linked to both diabetes and cardiovascular disease, its presence often signals a higher overall risk for heart-related complications. Like other vascular conditions, PAD develops gradually, meaning symptoms may be mild or intermittent at first, which can delay diagnosis and treatment if not carefully monitored.
Managing the combined risks of diabetes, heart disease, and related circulation problems requires a comprehensive and consistent approach. One of the most important factors is maintaining stable blood sugar levels, as long-term glucose control helps reduce damage to blood vessels and nerves. Regular physical activity also plays a key role by improving circulation, strengthening the heart, and supporting overall metabolic health. In addition, lifestyle choices such as avoiding smoking, maintaining healthy blood pressure, and managing cholesterol levels are essential in reducing cardiovascular risk. Medical check-ups and routine monitoring allow for early detection of changes in blood flow, nerve function, and heart health, enabling timely intervention when needed. For individuals with diabetes, regular foot examinations are especially important, as they can reveal early signs of circulation problems or injury before they become severe. Simple daily practices, such as inspecting the feet for cuts, swelling, or color changes, can make a significant difference in preventing complications.
Ultimately, foot health serves as an important window into overall vascular and cardiovascular health. Because the feet are often the first area to show signs of reduced circulation or nerve damage, paying attention to changes in this part of the body can provide early warnings of more serious underlying conditions. Recognizing symptoms such as pain, numbness, temperature changes, or slow-healing wounds allows individuals to seek medical advice before complications develop further. Early detection and proactive care can significantly reduce the risk of severe outcomes, including infections, tissue damage, or cardiovascular events. By understanding the connection between diabetes, heart disease, and circulation, individuals can take informed steps to protect both their immediate and long-term health.